As a pediatric clinician providing ADHD care, there’s pressure of managing patient and parent expectations, handling reimbursements, staffing your clinic, and making efficient use of your time.
By systematically reviewing and refining your clinical workflow, it’s possible to build a successful pediatric clinic that provides quality ADHD patient care whilst operating efficiently. From intake to follow-up, here’s how to make your pediatric clinic an ADHD success story.
Disclaimer – This blog is not intended as an exhaustive guide. ADHD is not a one-size-fits-all condition, and each patient’s experience is different.
The information should be used at your discretion and does not constitute medical advice.
How to build a high-quality onboarding process for your patients
Your intake process sets the tone for patient and parent experience across the ADHD patient journey. Getting intake right means making a great first impression with your new patient and also providing you with data required to register that patient and start the assessment.
Why is an effective onboarding process important?
A digital-first patient intake reduces your admin burden and is a user-friendly introduction to your clinic for patients.
A strong pediatric onboarding process balances consistency with personalization. Consistent workflows are scalable and promote patient equity. However, you will need to tailor initial consultations based on patient age. For younger patients, parents are at the center of the intake process, while for teens, more autonomy and patient input is beneficial.
Structure your intake process so you're gathering information from multiple sources. This is usually parents, teachers, and, where age allows, the patient too. This ensures data collected during patient onboarding aligns with DSM-5 criteria for observing ADHD symptoms in two or more settings (e.g., at home and in school).
How pediatric clinics can improve assessment quality
There are several steps you can follow to establish a high-quality assessment process for your pediatric ADHD patients.
Use multiple data sources during ADHD assessment
Rating scales, clinical interviews, and patient, teacher, and parent feedback are all valuable components of the ADHD assessment. However, subjective measures of ADHD symptoms are vulnerable to responder bias. Parents and teachers can also provide very different rating scale feedback on a child’s ADHD symptoms. These can make it difficult for you to accurately diagnose ADHD.
A multi-modal ADHD assessment reduces the overreliance on subjective data sources to diagnose ADHD symptoms. Adding a digital ADHD test to your pediatric workflow can help you cross-validate findings, identify reporting inconsistencies, track symptom change, and differentiate between ADHD and comorbidities.
Align your assessment workflow with ADHD diagnostic criteria
Data collection during assessment is critical, but you then need to interpret what that data tells you about a patient’s condition. The DSM-5 criteria are particularly useful here.
“Do your patients’ experiences align with the ‘real-world’ examples of ADHD in action?”
“Is there evidence of symptoms in more than one setting?”
“Were symptoms present before age 12?”
You will also want to consider if there is a consistent picture between subjective and objective data sources to allow you to reach a diagnosis.
Base your final diagnosis of ADHD pediatric cases on your clinical judgment
Developmental history and data from rating scales, interviews, and objective tests can all help to present a picture of a child’s symptoms and experiences. But it is your own clinical judgment that is the final step of the process.
Reaching a diagnostic decision can be difficult, particularly in borderline cases like girls with subtle symptom presentations or pediatric patients with comorbidities. So, it’s really important that your decision is supported by a full, consistent, and comprehensive workflow.
Explore tips on creating an ADHD-friendly classroom
Our educator checklist includes helpful tips for creating an ADHD-friendly classroom. Share it with parents and teachers of children with ADHD to better support their care journeys.
What makes an effective pediatric treatment plan?
Pediatric ADHD care often requires a more collaborative approach than adult ADHD care. Treatment of your patient will require involvement from parents and teachers, as well as the child themselves. Without collaboration, there is the risk of fragmented approaches to care, and treatments may not be consistently applied in school and at home.
Set patient and parent goals around information sharing and personalization of treatment to promote a healthy patient journey.
Parent-teacher training may also become part of the treatment plan. This includes behavioral interventions for parents and classroom management skills for teachers. It can lead to symptom reduction in children, improved academic performance, reduced parent stress, and better parent understanding of ADHD treatments.
Why is follow-up critical in pediatric care?
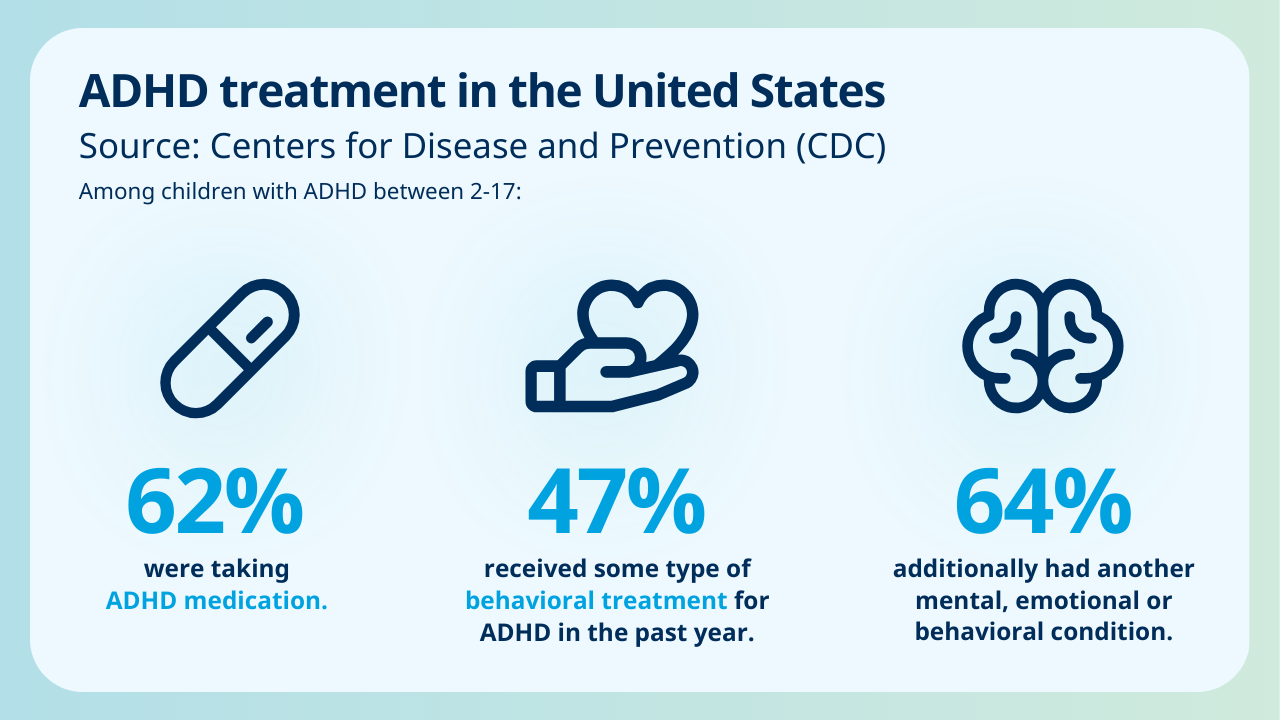
Studies have found low medication adherence in long-term ADHD care for children and adolescents. Patients continued with medication for an average of just under six months, and at 12 months, only 22.9% of patients still had good medication adherence.
Pediatric patients and families face several challenges, including cost, access to treatment, stigma, and difficulties in self-management of treatment. These can all contribute to non-continuation.
It’s important that your ADHD workflow supports long-term patient care. Regular scheduled follow-ups and systems of support between appointments, such as psychoeducation and secure messaging facilities, can all help. Key pinch-points such as transitioning from childhood to adolescence and the transition to adult services, a known drop-off point, should also be managed carefully.
What does a successful ADHD pediatric clinic look like?
Successful pediatric care is built across the patient journey. Structuring your workflow to ease intake, collect multiple data sources, align with diagnostic criteria, tailor treatment plans, and manage follow-ups can help you build a successful, scalable model of ADHD pediatric care.
To discuss adding objective testing to your clinic’s workflow, speak with one of our expert advisors by filling in the form below.
