The mental health awareness movement is making an impact online – ADHD is no exception. Many of you reading this will most likely have stumbled across more people (across all media) opening up about their experiences with mental health. Or, you might have come across hashtags on social media and messages such as #itsokaynottobeokay.
Although the thinking behind the phrase is well-intentioned, ‘people should be comfortable in speaking up when they’re not okay’, it raises some debate. For example, while it is positive that people talk about their challenges, is it really okay to not be okay for an extended time?
Do we need to see a shift in the message?
Rebecca Lawrence of The Guardian makes this point: “There are many well-meaning campaigns that encourage disclosure of illness; the problem is that they’re not always followed up by the resources necessary to actually help people”. The question then is, do we need to see a shift in the message? In his podcast, Life Lessons from Sport and Beyond, Simon Mundie and Clinical Psychologist Dr. Amy Izycky discuss how we might adapt “the narrative around mental health from ‘It’s okay not to be okay’ – true of course – to ‘it’s okay to do the work to be ok”.
With many mental health and neurodevelopmental conditions, the ‘work to be okay’ is multifactorial, and the best approach for ADHD specifically, according to the literature, is a combination of medication and behavioral intervention. Similar to other conditions, there is still a stigma around medication. The #PostYourPill campaign led by Dr. Alex George, Youth Mental Health Ambassador for the Department for Education, led to an outpouring of social media posts of people sharing the medication they take for various mental health conditions and explaining why they take them. This has unquestionably had a positive impact on challenging the negative stereotypes related to people taking medication to support their mental health. Among the social media posts were many sharing their use of medication for ADHD – again sharing an important message that, for some people, medication has a real impact on their symptoms.
This campaign also touches on something important – treatment compliance. Adherence to treatment among those with ADHD is low, perhaps, in part, due to the fact that a common symptom is forgetfulness. Plus, there is often some reluctance to take medication given the stigma and misinformation around stimulant medication.
Take the example of the online media publication Vice comparing Adderall to methamphetamine – a commonly pedaled and incredibly unhelpful analogy with one being a prescribed, FDA-cleared, treatment and the other being an uncontrolled and highly illegal street drug.
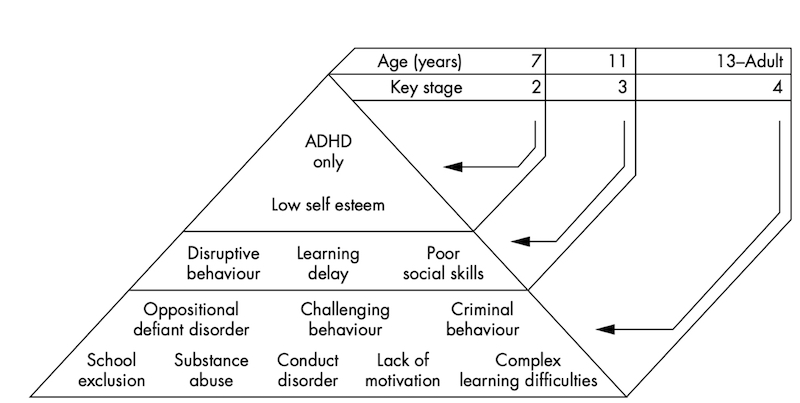
It is worth highlighting that ADHD is a debilitating disorder that in many cases continues into adulthood which impacts many aspects of someone’s life and these change as individuals get older.
Is awareness and the shared experience enough?
Many people go through their life thinking something is wrong with them and do not know why. For many people, a diagnosis was the last piece of the puzzle the start to finally understand themselves. When people do receive a diagnosis, many are left feeling ‘so what now?’. Many start developing coping mechanisms and learning how to manage their ADHD. Some do lots of research and find that connecting with others (online and offline) who also have ADHD helps, finding out that all those traits you thought were individual to you, or picked on for, are shared by thousands of others.
This leads directly back to the fundamental point we’re making here. Is awareness and the shared experience enough? For some, it might be, depending on the environment you’re in, the work you have, and the demands of life. ADHD certainly doesn’t prevent you from succeeding educationally or vocationally, but for many people, ADHD can put a significant strain on many aspects of their life and research shows that treatment is the best course of action in these cases.
Research shows children with a diagnosis of ADHD that are treated have better educational outcomes than children with just a diagnosis of ADHD. Additionally, research featured in The Archives of Pediatrics and Adolescent Medicine shows that there is no benefit in identifying children with ADHD without then providing them with extra support and treatment. The researchers suggest this may reflect the adverse effects of labelling, i.e., children may be treated differently after having received an ADHD ‘label’ at a young age. This raises several problems, but most concerning is that children not only have to deal with difficult ADHD symptoms but may also suffer the consequences of the stigma and shame surrounding ADHD.
There is no shortage of evidence showing how un-managed/un-diagnosed ADHD can severely impact an individual, their family, and society – showing how important a joint effort to identify and support a child with ADHD is. Ultimately, it is so important that we are having frank conversations about ADHD and mental health as a whole, and for the best results, it must be followed by action, both from providers and patients. For ADHD specifically, we must find ways to support those who want to act, specifically targeting the stigmas (which sadly still exist) and adherence – making the most of technology to help patients get to their appointments and take their medication if prescribed. Getting an objective look at symptoms and how they can improve with medication is also paramount to increasing patient understanding of their symptoms, and how medication may help.
Learn more with our objective ADHD tests.
