Eating disorders (EDs) and ADHD often co-occur, and patients can present with overlapping symptoms. Impulsivity, binge eating, and attentional difficulties are common for both conditions, making diagnosis and treatment more challenging.
Manchester NHS Foundation Trust (MFT) Community Eating Disorder Service (MFTCEDS) incorporated objective ADHD testing into its patient journeys. This has enabled them to treat more patients within their workflow, without having to refer out. It aided in streamlining care and improving overall patient outcomes.
Is there a link between ADHD and eating disorders?
Multiple studies have highlighted a connection between ADHD and eating disorders. Here are some of the findings:
- Children with ADHD are at increased risk for disordered eating
- Adolescents, young adults, and adults with ADHD are at risk for both disordered eating and eating disorders
- Girls with ADHD are 3.6 times more likely to develop eating disorders than those without
- 40% of patients accessing the CEDS service in Manchester are neurodiverse (up from 20% pre-pandemic)
What eating disorders are associated with ADHD?
There are several known links between ADHD and specific types of eating disorders, including bulimia nervosa, binge eating, and overeating:
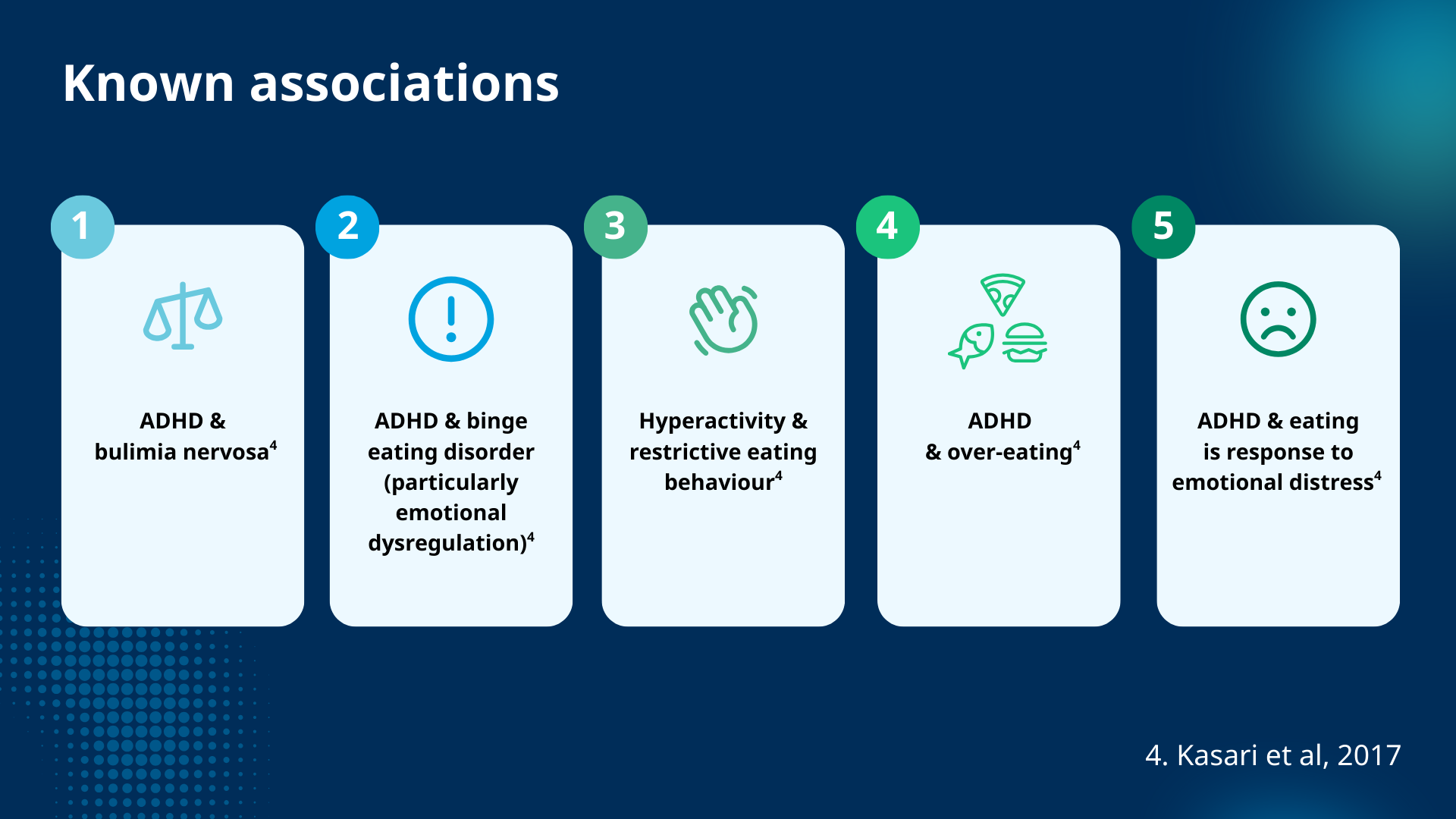
Explore the link between ADHD and eating disorders in more detail in our Rethinking ADHD podcast.
The challenge
Overlapping symptoms can make diagnosis difficult and treatment journeys complex
A systematic review of Anorexia Nervosa, Avoidant/Restrictive Food Intake Disorder (ARFID) and Bulimia Nervosa, showed a co-occurrence rate ranging from 7% to 48%.
Historically, neurodiverse patients presenting to the MFTCEDS team were referred to CAMHS. This resulted in significant delays in assessment (with wait lists up to 1.5 years for CAMHS) and a more siloed approach to treatment.
To tackle their issue, the team decided to start treating neurodiverse patients internally.
The solution
Integrating objective ADHD testing tools to strengthen assessment accuracy and patient care
MFTCEDS developed a 'neurodiversity pathway' for patients presenting with eating disorders and evidence of neurodiversity. Patients on this workflow now complete a digital ADHD test during the assessment process.
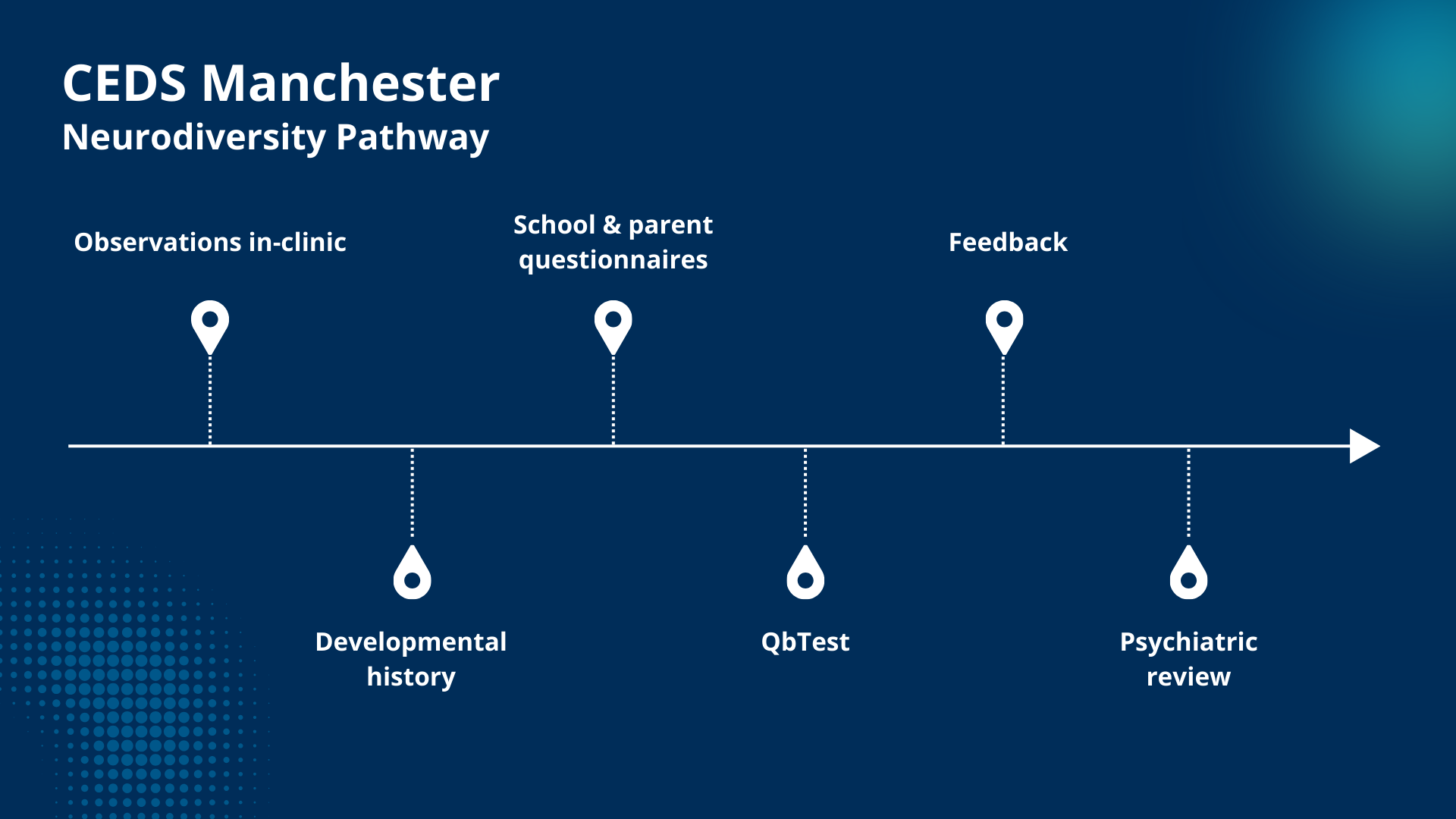
The objective test provides clinicians with a measure of the patient’s hyperactivity, impulsivity, and inattention compared to same-age and same-sex at birth control data for individuals without ADHD.
Alongside this, the CEDS team collects information on neurodiversity symptoms from school staff and parents. When combined, this data can help clinicians to diagnose or rule out ADHD and inform treatment decisions.
"Implementation of our own robust ADHD/ND assessment pathway including Qbtesting has enabled us to correctly diagnose and treat underlying ND conditions which would previously have not been identified and potentially impacted effective treatment."
- Molly Caine, Service Lead
Objective testing is sometimes repeated during the treatment phase. It can help clinicians with ADHD treatment titration and may also be used to check dosage adjustments when a patient’s weight changes.
The impact
Objective data helped inform treatment decisions and streamline care
The introduction of Qbtesting in their Neurodiversity Pathway helped:
- Screen for ADHD in patients presenting with eating disorders
- Inform treatment decisions with reliable, data-driven insights
- Monitor progress and medication effects during treatment or weight restoration
Before digital ADHD testing, patients would not have received ADHD treatment from CEDS and instead had to wait for a CAMHS referral. The addition of objective testing enables earlier identification and quicker access to appropriate treatment.
Key takeaways
Integrating ADHD testing into eating disorder care
In many cases, a positive ADHD diagnosis facilitated by Qbtesting led to patients being treated for the condition, which in turn addressed their eating disorder symptoms.
“Our patient (17-year old female) presented with restriction and weight loss. She was diagnosed with anorexia nervosa and struggled to restore weight. Five months after initial assessment, ADHD was diagnosed using objective testing and we began treatment leading to symptom improvement and weight restoration. There were no residual ED behaviors.”
Integrated care models reduce delays and improve patient outcomes. A more personalized treatment plan also ensured interventions were specifically targeted to patient needs.
