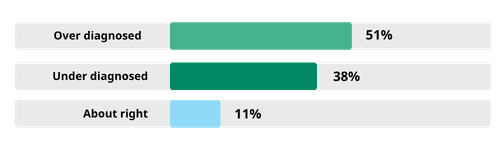
Last month’s Rethinking ADHD subscriber poll produced a striking result: over half of clinicians felt that ADHD is over diagnosed, compared with 38% who felt it is under diagnosed, and 11% who believed rates are about right.
This contradicts what official ADHD prevalence figures show. That’s not to discount direct clinical experience during a period of unprecedented service demand post pandemic – these responses highlight a persistent gap between what’s seen in practice and what years of epidemiological data, diagnostic history, and major government reviews show.
That evidence shows a shift in the demand for assessment, not widespread ADHD over diagnosis. It instead points to a more complex reality: rising recognition, persistent under diagnosis in key groups, and clinical workflows that aren’t designed to manage diverse, complex presentations.
Prevalence has remained stable, demand has not
Research has place ADHD prevalence at approximately:
What the data consistently shows is that ADHD prevalence itself has remained broadly stable over time – as shown by the UK government’s March 2026 interim review, which was supported by international population-based research. What’s changed in recent years is how often ADHD is recognized and assessed.
In the US, there are higher prevalence rates than most countries. A study in 2022 showed 1 in 9 children were diagnosed with ADHD. Yet, Black, Asian, and Hispanic children are less likely to receive a diagnosis.
With persistent under diagnosis and later diagnosis in certain populations (including women, adults, and some ethnic and socio-economically disadvantaged groups), this points to long-standing differences in recognition and access alongside ongoing gaps in who is identified and when.
Why ADHD feels over-diagnosed in clinical practice
The idea that ADHD is over diagnosed is understandable. However, for a long time ADHD was narrowly viewed as a childhood condition characterized by overt hyperactivity in young boys and as a result, entire populations were systematically overlooked.
ADHD has become more visible than ever on social media and in the wake of the pandemic. Clinicians are now seeing a surge of referrals from patients who actively identify with its symptoms.
The increase in diagnosis is consistent with how ADHD is now defined and recognized, rather than a loosening of clinical standards.
Change in diagnostic guidance from 2013 (the transition to DSM-5):
Adult ADHD
-
- The evolution of the ADHD construct into its current characterization in DSM-5 reflects more than two decades of increased awareness that ADHD is not limited to childhood and adolescence.
- ADHD has been formally established as a lifespan neurodevelopmental condition.
- Introduction of adult diagnostic criteria, making adult diagnosis more accessible and accurate.
Functional impairment
-
- Functional impairment is required for an ADHD diagnosis in the DSM-5, however the time frame and definition of functional impairment is ambiguous.
- Careful evaluation of co-morbidities is essential, however is also challenging to isolate and assess separate to other conditions like anxiety/depression.
- Differences in clinician judgment are often interpreted as over diagnosis, when they more accurately reflect the condition’s heterogeneity.
Awareness around other conditions is changing
Increased diagnosis does not necessarily mean increased prevalence. In healthcare, it’s usually seen as a positive thing and often reflects better screening, for example in colon cancer and HPV.
Systems built around diagnosis, not need
Diagnosis has become a gateway to support in systems not designed to manage the full spectrum of neurodevelopmental need.
This creates bottlenecks and long waiting lists, pressure on clinicians to “diagnose or discharge”, and the illusion of over diagnosis, when the deeper issue is the clinical workflows in place.
Why clinicians could benefit from reframing ADHD
The goal isn’t to persuade clinicians to diagnose ADHD more freely, but to:
- Maintain high diagnostic standards.
- Avoid dismissing ADHD due to discomfort with its increasing visibility.
- Recognize that improved detection is not diagnostic inflation.
- Balance healthy skepticism with evidence-based decisions.
Using standardized objective tests in your ADHD clinic
Thank you to everyone who participated in the poll. These conversations matter, and they make us better clinicians when we’re willing to challenge our own assumptions as rigorously as we challenge diagnoses.
Real-world presentations and accurate diagnosis is complex. Objective testing can help to standardize your clinical workflow with robust data and positive patient outcomes. Get started with QbCheck.
